This may seem like a totally redundant question as it is so obvious on the face of it that bereavement is what happens when someone close to you dies. However, it is worth exploring more.
The Oxford English Dictionary defines ‘bereave’ as to be deprived of a close relation or friend through their death. The origin of the word ‘bereave’ is from the old english word ‘bereafian’. The original sense was ‘deprive of’ in general; reave – to rob of something by force; steal. To be bereaved is to be sorrowful through loss or deprivation; bereft of hope.
From these dictionary definitions, we can see that bereavement, in addition to grief, also carries the sense of something being stolen from us, a deprivation, and sorrowful suffering. A sense of injustice can pervade – Ernest Becker describes in detail the struggle that humans endure in facing their and their loved one’s mortality. There are a number of different lenses we can use to look at the experience of grief from the tension between being in the world and withdrawing from it1; to the dual process model of grief whereby we oscillate between loss and restoration2,3 feeling like we are in a spiral of confrontation and avoidance of loss; to Worden’s tasks of mourning4 and Tonkin’s Growing around Grief model5,6; there are phases of grief 7and dimensions of loss8 including an acknowledgement of the impact of loss on our identity according to Susan Le Poidevin’s Multidimensional Model.9 These different models can help intellectually to understand what we are going through and to normalise what is happening. There is also something very useful in understanding the experience specifically for medical students.
Specifically, given that students are embedded in a demanding university course, there is a tension or dilemma between whether to take a break and care for their loved one or to grieve; and whether or not to carry on with course albeit perhaps with provisions to help cope; or at least have an understanding of the rollercoaster of emotions students will go through and which may be triggered by the course material, clinical placements and/or patients and their families. That is, when studying medicine, students are embedded in the very field that their loved one may be entering and then leaving permanently. There is every chance that medical students will come across material and patients that will remind them of their loved one. If the experience is not processed, this may mean that students suffer later on in an accumulation or outpouring of grief or a frantic repression at all costs. What follows are some descriptions of the more subtle aspects that do not always get spoken about of the experience of loss whilst at medical school.
Students can feel caught between competing demands of the course, their family and their own mental, emotional and physical needs. Feeling caught can manifest in guilt or shame which further the sense of being trapped in the experience. The trapped feelings can be exacerbated by difficult relationships within the family, or between the student and the loved one who has died making grief more complicated10. As well as the dual process of confronting and avoiding the loss of a loved one, students are also experiencing a dual process of task focused coping and emotion focused coping11. A useful self-help guide is published on the NHS Scotland website12.
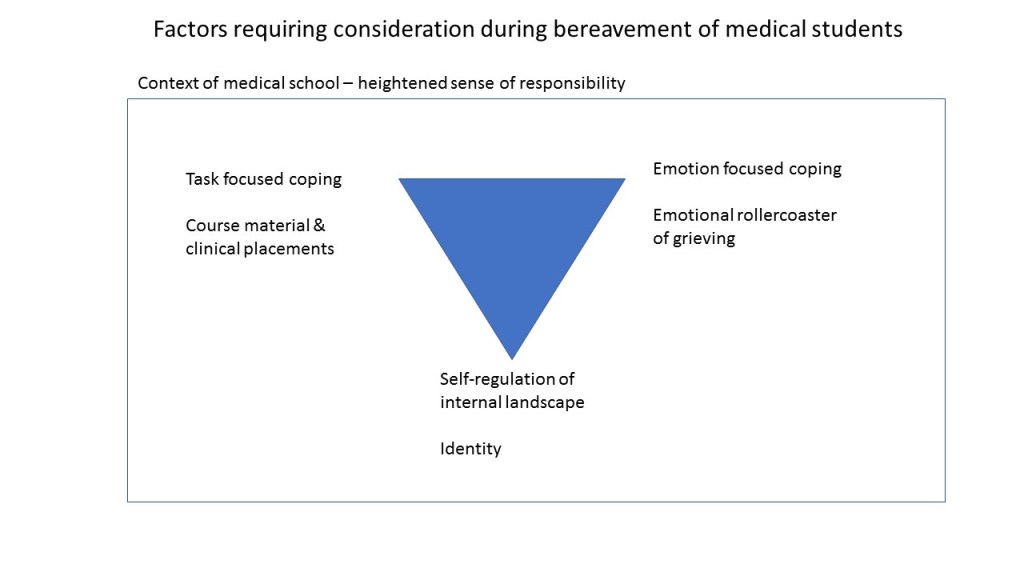
The intensity of the feelings and the frequency with which students experience changes between being task or emotion focused or just trying to manage their own internal landscape can depend on how acute the loss is and if there is someone trustworthy you can talk to, if you are able. The fluctuations in themselves can be experienced as distressing and students can long for a return to ‘normal’; whatever that may mean to them.
Many students feel isolated with their grief and this has been particularly notable during the pandemic. This isolation makes it harder to navigate through waves of emotion, trying to get work done, and coping with the reality of losing a person who has been an anchor in your life. At times like this, it can feel as though you are cut loose without any anchors, floating in a void or abyss; particularly if there are troubled relationships within the rest of the family meaning they are unable to act as stabilizers. The importance of having a trusted person you can talk to and who will listen cannot be underestimated. Having an awareness of these sorts of feelings and experiences can help students to know that these experiences are part of the grieving and suffering journey and can also help to manage the peaks and troughs of that journey. Even when these experiences cannot be described explicitly in words they are still part of the experience of grieving. Some pictures and poems follow to illustrate these experiences and to perhaps help students piece together their own trajectory.

The Unsayable

The Abyss
Suffering itself is described as wordlessness, loss and seeing yourself on the wrong side of an abyss that separates you from life13. The experience of suffering can seem as misty or intangible or unsayable. Making use of words, images and poems to write a letter or draw a picture or reflect on an image that has meaning for you are all ways to make connections between your experiences which can help process the grief and restore you to yourself. By restoring aspects of your experience, you are starting up a conversation with yourself about your loss and suffering. This is important because when we lose someone we can become paralyzed by that loss as we lose our habitual ways of going about our life and as yet have nothing to replace them. The sense of losing our internal maps, as represented by the other person, can be a source of distress as they are our guide to being in the world. With time we will put together a map that can encompass the loss.
Sometimes the paralysis can be from not being able to face a difficult situation with the loved one. The film ‘A Monster Calls’ (2016)14 shows the struggles that a boy goes through with his mother’s terminal illness and how this is symbolized by the fear of falling into the abyss. All of these different aspects of the grieving process are natural human reactions. However, by not talking about them, we can fear them, and so set up a secondary process of anxiety about the experience. These are some of the aspects of the internal landscape that people who are grieving must navigate as well as learning a new identity in the face of a loss or absence. Coupled with attending a demanding course that may trigger emotional waves of grief due to the very nature of the course, you can see that this is an intense process and one which requires the utmost self-care and compassion. We are experiential as well as narrative beings. Talking about experiences and normalising them can lessen the isolation that students feel around bereavement.
References
- Papadatou D. A proposed model of health professionals’ grieving process. OMEGA. 2000; 41(1): 59-77Papadatou D. A proposed model of health professionals’ grieving process. OMEGA. 2000; 41(1): 59-77.
- Stroebe M, Schut H. The dual process model of coping with bereavement: rationale and description. Death Stud. 1999 Apr-May;23(3):197-224. doi: 10.1080/074811899201046. PMID: 10848151.
- https://mindfulnessandgrief.com/dual-process-model-of-grief/
- Sheila Yousuf-Abramson (2021) Worden’s tasks of mourning through a social work lens, Journal of Social Work Practice, 35:4, 367-379, DOI: 10.1080/02650533.2020.1843146
- https://www.cruse.org.uk/understanding-grief/effects-of-grief/growing-around-grief/
- Lois Tonkin TTC, Cert Counselling (NZ) (1996) Growing around grief—another way of looking at grief and recovery, Bereavement Care, 15:1, 10, DOI: 10.1080/02682629608657376
- Bowlby, J. and Parkes, C. (1970) Separation and Loss within the Family. In Anthony, E.J. (ed.) The Child in His Family. New York: Whiley.
- https://www.cruse.org.uk/wp-content/uploads/2021/09/94149-After-the-death-of-someone-very-close.pdf
- Susan Le Poidevin’s Multidimensional Model.
- Shear MK. Grief and mourning gone awry: pathway and course of complicated grief. Dialogues Clin Neurosci. 2012;14(2):119-128. doi:10.31887/DCNS.2012.14.2/mshear
- Snyder CR. 1999. Coping: the psychology of what works. Oxford University Press: Oxford.
- https://www.nhsinform.scot/illnesses-and-conditions/mental-health/mental-health-self-help-guides/bereavement-and-grief-self-help-guide
- Devisch I., Vanheule S., Deveugele M., Nola I., Civaner M., Pype P. 2017. Victims of disaster: can ethical debriefings be of help to care for their suffering? Medical Health Care and Philosophy; 20:257-267.
- https://www.imdb.com/title/tt3416532/


